Read More
Daily 10-minute "zero-sweat fat loss method" can reduce waistline by 5cm
14-05-2026 12:00 HKT
82-year-old former senior police officer found dead at Sai Kung home
14-05-2026 18:46 HKT
Many parents think their child's snoring is a sign of "sleeping soundly," but this could be a warning sign of sleep apnea. As an ear, nose, and throat (ENT) specialist, I often see parents in my clinic seeking help for their child's developmental delays or poor concentration, only to find the culprit is obstructive sleep apnea. This condition not only affects sleep quality but can also alter a child's facial appearance.
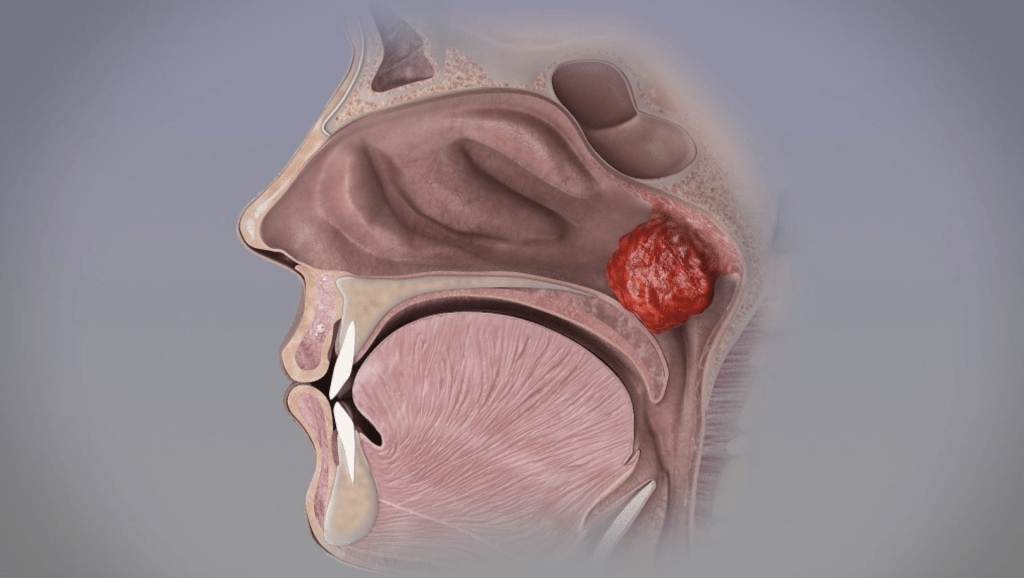
Pediatric obstructive sleep apnea (OSA) is a sleep disorder where patients experience pauses in breathing or shallow breathing during sleep due to upper airway obstruction. The most common cause is enlargement of the tonsils and adenoids, which block the airway. Other contributing factors include obesity, allergic rhinitis, and craniofacial skeletal abnormalities. Patients can experience dozens of micro-awakenings per night, leading to fragmented sleep and repeated episodes of brain hypoxia.
Long-term untreated sleep apnea in children not only affects their health but also impacts facial development, leading to what is known as "adenoid facies." Because the adenoids in the nasopharynx are enlarged, children are forced to breathe through their mouths chronically. This disrupts the balance of facial muscles and affects normal craniofacial skeletal development. Characteristics include:
Recent studies indicate that the prevalence of adenoid hypertrophy in children is approximately 49.7%. Mouth breathing, malocclusion (poor teeth alignment), and abnormal facial development can form a vicious cycle, exacerbating each other. If parents notice these features in their child, they should seek medical advice promptly.
For sleep apnea caused by enlarged tonsils and adenoids, adenotonsillectomy is the most common and effective treatment. Many parents worry whether their child is too young for surgery. Clinically, children with obvious symptoms are candidates for surgery. Research confirms that timely and appropriate surgical intervention can significantly improve a child's health and academic performance. A 2025 pediatric study published in the US showed that children with mild sleep-disordered breathing who underwent adenotonsillectomy had a 32% reduction in overall healthcare utilization and a 48% reduction in prescription medication needs within one year.
However, surgery is not the only option. For mild cases, especially in children with smaller tonsils, watchful waiting may be a reasonable choice. Treatment plans must be personalized, depending on the location and severity of the airway obstruction. Some patients may also require orthodontic treatment or orofacial myofunctional therapy.
If pediatric sleep apnea is not diagnosed and treated promptly, chronic hypoxia can affect brain development, leading to daytime sleepiness, poor concentration, learning difficulties, and even behavioral problems. Long-term, it also increases the risk of developing hypertension, heart disease, and metabolic disorders. Therefore, if parents notice habitual snoring, breathing pauses during sleep, mouth breathing, or nighttime bedwetting in their child, they should seek an ENT specialist's opinion as soon as possible to seize the critical window for correcting facial development and improving overall health.
Download The Standard app to stay informed with news, updates, and significant events: